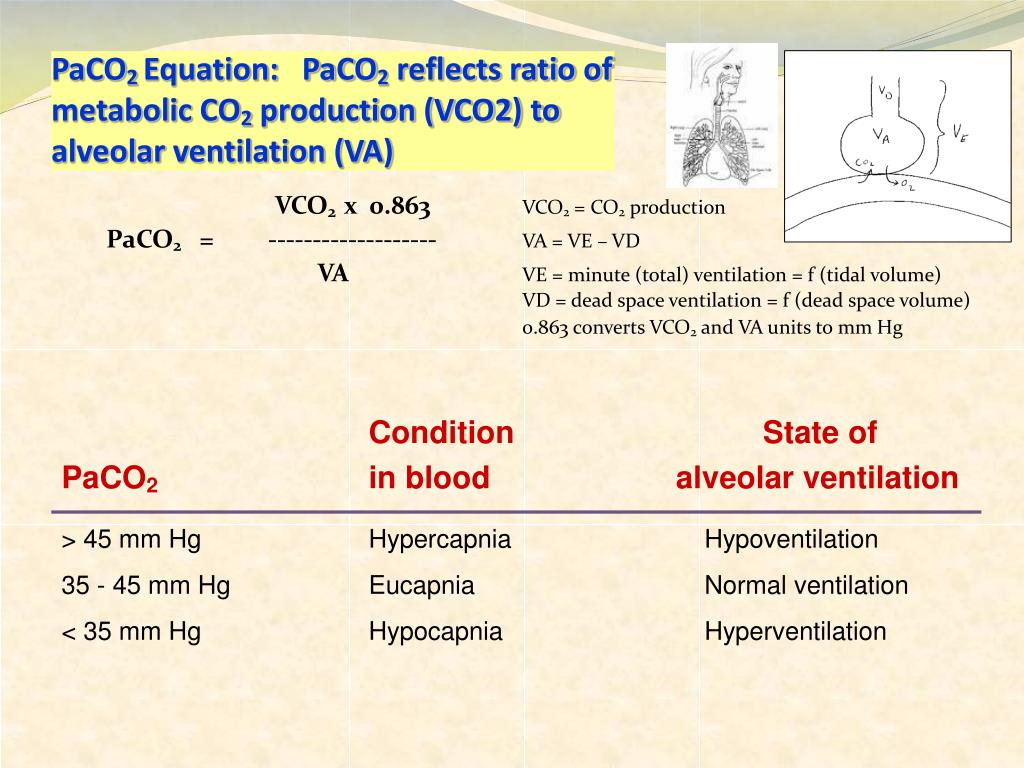
Depending on the disease condition, additional mechanisms that can contribute to an elevated physiological dead space measurement include shunt, a substantial increase in overall V'A/Q' ratio, diffusion impairment, and ventilation delivered to unperfused alveolar spaces. For the range of physiological abnormalities associated with an increased physiological dead space measurement, increased alveolar ventilation/perfusion ratio (V'A/Q') heterogeneity has been the most important pathophysiological mechanism. PEEP is routinely used in mechanical ventilation to prevent collapse of distal alveoli, and to promote. 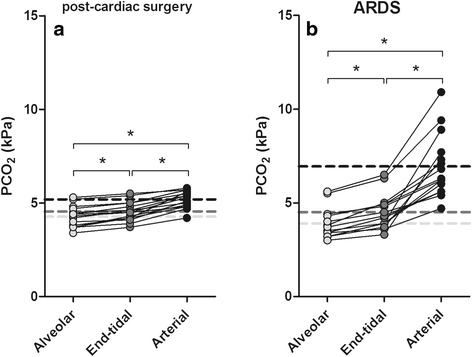
PEEP acts to distend distal alveoli, assuming there is no airway obstruction. Although a frequently cited explanation for an elevated dead space measurement has been the development of alveolar regions receiving no perfusion, evidence for this mechanism is lacking in both of these disease settings. Positive End-Expiratory Pressure (PEEP) is the maintenance of positive pressure (above atmospheric) at the airway opening at the end of expiration. An elevated physiological dead space, calculated from measurements of arterial CO2 and mixed expired CO2, has proven to be a useful clinical marker of prognosis both for patients with acute respiratory distress syndrome and for patients with severe heart failure.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
